Dialogue between doctor and patient
-
the nine steps from theory to application
in daily medical practice
The reader who has been patiently
following, and is now prepared to change his approach (that is to talk
to his patient with real understanding) will probably not without uneasiness
ask how he can possibly translate his goodwill into reality under the pressure
of daily clinical practice. Many terms are probably whirling around in
his brain without clear order or classification: open and closed techniques,
active listening, empathy, as well as first and second order reality. He
is probably also wondering, how, with the best will in the world, the time
available can be enough to allow him to speak to his patients in any other
way than he has always done.
The way to apply theory
in clinical practice is best accomplished by using single steps
systematically. The following scheme should allow the reader to pursue
this goal in nine stages. He is free to decide himself how long each will
take. Initially he should perform a critical analysis of dialogues
which he has followed previously, especially with regard to the quality
and efficiency. Further steps are involved in the learning process about
discussion, with a new orientation of standpoint, as well as one's reaction
to the patient. The final stage is the most difficult, as the ballast
of previous perceptions about the nature of reality has to be thrown overboard,
in order to recognize that it is only possible for a doctor to communicate
(in the true meaning of the word) with his patient when a mutual reality
has been established.
If the reader is prepared
to walk this path, he should go about it with a quiet and relaxed manner.
All of the steps can be integrated "en passant" in daily clinical practice
and do not require an additional time expenditure. The further the reader
proceeds, the more often he will accomplish what he only occasionally experienced
previously, and that is pleasure. Pleasure because he is experiencing
what he can accomplish with the most important (but also most neglected
physician's instrument) which is that of speech. The doctor's discourse
becomes a treat to treat!
| top |
 |
|
First step - a critical
self-appraisal
More than anything else, the
first step requires a well-developed ability of self-criticism. It should
allow an honest answer to the question: "Just how many of my discussions
with patients are unsatisfactory for the patients, for myself or for us
both?" The normal burden of the doctor's working day is often so great
that the doctor is happy enough just to manage to perform all that is required
of him. The question as to whether all the conversations were good, and
satisfactory for both parties, can easily be dismissed as unimportant.
However unsatisfactory discussions do not, as it were, lie quietly under
the carpet.
If the patient is
dissatisfied, this discontent can be expressed in several ways. Only in
very rare cases will the patient say directly that he was disappointed
with the consultation. This dissatisfaction is more likely to be expressed
in a non-verbal form. The result of an unsatisfactory conversation is likely
to manifest itself in the behaviour of the patient who reacts with
aggression, rejection or anxiety. He comes back with the same queries.
Compliance is unsatisfactory. He refuses useful investigations and suggestions
for therapy. He gives the impression that he does not understand us, and
that we have not understood him. He displays "difficult" behaviour. He
repeatedly comes with the same complaints, or perhaps never comes again.
Obviously there are some
conversations which the doctor well knows to have been a failure.
However in many more cases he will be aware only subconsciously that he
has conducted unsatisfactory consultations.
Unsatisfactory conversations
with patients have a particularly stressful effect; they soon lead to tiredness,
which expresses itself by irritation and aggression. They create the impression
that one does not want to see the patient again in the near future. If
he does come again, one sighs and attempts to subdue the sense of antipathy.
After the discussion, one is left with the feeling that the whole of the
interview consisted of shots in the dark. Nothing appears to have changed;
in fact just the opposite - the situation has become more consolidated
or the dialogue has produced further difficulties rather than solving the
original problems. The treacherous deception is that the conversation which
is unsatisfactory for the doctor, can insidiously be quite satisfactory
(on a superficial level) for the patient, as it may have been "reassuring",
without him being aware that all mentions of the actual problems were suppressed,
deflected or minimized.
Throughout several days,
ask yourself after each conversation if it was satisfactory; and if it
was unsatisfactory, was it so for the patient, for yourself, or for both
participants in the discussion. The results of this "internal self-analysis"
can be decisive in motivating you to conduct consultations differently
in the future. A further method of assessing the quality of your own technique
is to ask colleagues for their critical opinion. Finally, it can be very
helpful to record the conversation on video, provided that the patient
does not object.
| top |
 |
|
Second step - listening
to yourself
Listening to what one actually
says is also an exercise in self-criticism, which can at the same time
become the starting point for assessing if, and to what extent, it is necessary
to improve one's techniques of leading discussions. The following points
should be borne in mind when critically listening to oneself:
Is my questioning technique
adequate and effective? Am I clearly showing empathy? Am I actively
listening? Do I make room for pauses in the discussion and am
I able to tolerate them and to interpret their significance correctly?
What sort of terminology am I using? Is there "communication noncommittalism"?
How often do I use impersonal terminology (such as that prefaced by "one",
"it", "we"), "Yes, but ...", undefined qualifications, generalizations,
exaggerations, duplicity (Trojan horses) or "killer phrases"? Does my way
of talking produce anxiety? Do I use refusal techniques (deflection,
evasion, minimization, incapacitation)?
Having looked at these aspects
of speech, it is important to perform an analysis of the content.
Was the conversation appropriate to the particular goal set for it? For
example, was it possible to motivate the patient? If the patient was anxious,
was the conversation aimed to deal with it? Was the "difficult" patient
accepted and included in the conversation? Were there conflicts present,
either in the subjects chosen for discussion or in the doctor-patient relationship,
and was it possible to change an insoluble conflict situation into a problem
solvable by means of discussion? Did the discussion take into account the
differences encountered if the patient is old or chronically sick? Were
the requirements of both the patient and of the team met during the ward
round? Did the discussion with the patient on the intensive care ward take
into account his need and difficulties with communication? Were conversations
with seriously ill or dying patients in essence genuine? Did the discussion
cease if the patient posed questions, even indirectly, about the reason
for illness or his being ill, or about God, or about what happens after
death?
| top |
 |
|
Third step - optimizing
the setting of the discussion
Even though willingness to conduct
good dialogue is present, the setting and environment can interfere with
satisfactory conversation. Experience shows that the setting of a medical
interview, whether in general practice or in hospitals, is often criminally
neglected. Conditions which could not be tolerated by a public authority
(or bank or airline company) are taken for granted in medical practice.
However the setting of the interview largely decides on the fate of the
discussion.
Watch out for the following
points:
Is your discussion as uninterrupted
as
possible?
Are disturbances, caused
by colleagues or assistants, telephone, intercoms, or other patients, minimized
or kept under control?
Is the place where
the discussion takes place appropriate (no corridor discussions, no standing
in the doorway)?
Are the distances
and seating correct?
Is the timing of
the conversation correctly chosen (for example, a cancer patient should
not be given the diagnosis in the evening, and a positive HIV result should
not be discussed on a Friday afternoon)?
Are obvious signs of hectic
activity and time-pressure avoided?
Overall, is the climate
suitable for a discussion?
| top |
 |
|
Fourth step - learning
to actively listen and reflect
An important sign of a good
doctor is that he has a good listening technique. This is the most
important skill that a doctor uses during interviews with patients. So
now test yourself to see whether, in general, you are a good listener.
Make it clear to yourself that you will often achieve more by active listening
than by good questioning technique.
Watch your behaviour during
conversations: do you tend to cut your patients short?
Are you able to cope correctly
with pauses in conversation? Do you allow enough pauses (time
for thought, communicative pauses) to encourage the patient to speak more?
Do you know the various reasons for pauses which inhibit or block discussion?
Are you able to tolerate breaks or silence during a conversation?
Active listening and reflection
(mirroring) especially by verbalization of emotional experiences are very
intimately related: the ideal drive for perceptive discussion is the integration
of listening and expressing understanding.
Next, observe which are the
basic
conditions for active listening:
Interest in the subject,
being prepared to listen, ability to hear and ability to be "completely
present".
Let your partner in conversation
know, without any doubt or misunderstanding, that you are truly and completely
intent on hearing what he has to say (readiness to listen). It is the interlacing
of speaking and active listening which forms the basis of successful discussion.
Never
interrupt your partner, as interruption is the absolute opposite of
active listening, and a prime destroyer of discussion. If at first
you become uncomfortable whilst actively listening, feeling that you should
not take as much time over this, you should remember that experience has
shown just the opposite: active listening saves time, inattention costs
time.
| top |
 |
|
Fifth step - recognition
of all messages in a signal
Rid yourself of the preconception
that a signal only contains one message (factual content). Consider
that speech is more than something that takes place when two computers
communicate: any statement can contain up to four messages:
| 1. |
Factual
information |
| 2. |
Self-revelation |
| 3. |
Relationship
(contact) |
| 4. |
Appeal |
Attempt to examine the statements
of your patients systematically, using the following four questions:
| 1. |
What
is the factual content of the statement? |
| 2. |
What does it
show me about the person with whom I am speaking? |
| 3. |
What is he trying
to express about me and/or our relationship with this statement? |
| 4. |
Is he trying
to achieve something, and if so, what? |
The most common mistake is
that the message heard is only "factual information", and that the possible
message about the relationship remains unheard. Check therefore what the
true major message actually consists of. Develop an ear for hearing
if the statement contains an implicit as well as an explicit message.
Do not forget that silence
represents a special form of signal on the part of the one who says nothing,
and that it can contain all the messages that are contained in the spoken
statement. Check whether one or other of your "hearing ears" is larger
than the other; it is usually women who tend to listen with a particularly
sharp "relationship" ear, whereas men tend to receive reports with their
"factual" ear. Always make it clear that you can work with all the messages
you receive; they are tools. Do not forget that while communication is
being carried out on the reporting level, communication is also proceeding
on the meta-level in the sense of implicit metacommunication. In
other words, be aware of the "that's what is meant" part of a signal.
| top |
 |
|
Sixth step - ability
to empathize
Empathy is a comer stone
of the understanding discussion. It is a bridge which leads from one's
own perception of reality into that of the patient, and allows mutual
reality to be found. Next: do not be afraid to use an empathetic approach!
You will gain at least as much as you have to put in. Be clear that empathy
should not be mistaken for sympathy, emotional involvement, fellow-feeling
or identification with the patient. Think about the definition of empathy:
"Empathy means to draw as completely and closely to the experience of the
other, as though it were one's own, never once losing the "as if" status.
If this "as if" status is lost, identification has taken over from empathy.
If you find it difficult
to behave empathetically, you should remember that for most doctors, the
desire to assist the suffering was decisive in the choice of becoming a
physician. Later experiences and self-protective mechanism often prevent
the realization of this original desire.
Further take into consideration
two
major hurdles that can prevent empathy. One is the need for "emotional
neutrality" and the other, the need to dominate. The "genuineness" of your
conversations with your patients is a good criterion for judging whether
you are capable of empathy.
| top |
 |
|
Seventh step - learning
to question and to stimulate questions
Now that you are more clearly
aware of the possible pitfalls in conducting consultations; that you have
created an atmosphere which in optimal for yourself, and are in a position
to listen actively; that you are able to receive information from more
than what is said, and to behave empathetically, you are now in a position
to utilize your discussion technique and to learn the art of questioning.
This involves differentiating between open and closed questions
and being clearly aware of the advantages and disadvantages of each. Closed
questions are probably better for obtaining immediate and objective information
rapidly; they are less useful for initiating or deepening discussion. Open
(non-structured) questions are appropriate for opening a discussion and
for delving into a particular area. Semi-structured ("serving men" questions)
are appropriate for throwing light on specific points.
Your questioning technique
is good when you succeed in stimulating the patient to describe in his
own words what it is that moves or troubles him. A metered number of
sounding, catalogue and reflection (echo) questions can help. Systematically
reject
inappropriate questioning techniques whilst steering the conversation.
These include leading, double and confrontation questions (unproductive
questions) together with the complete range of forbidden questions (snare/trap,
curiosity, judgmental, aggressive and flowery [rhetorical]). The more you
succeed in improving your questioning technique, the more you will acknowledge
that the good question is already a part of therapy. However, even
when your questioning technique is optimal, you should not lose sight of
the fact that active listening often brings more to light than any question,
however discerning.
Finally do not forget to
consider the questioning behaviour of your patient. What are his
real
reasons for asking (need for information, desire for attention, cry
for help)? Why does he ask that at this particular moment? Is there
a question behind the question? Why does the patient repeatedly
ask the same question? And are you alerted if the patient does not ask
anything (anxiety, time pressure, barriers to communication, incompatible
realities)?
| top |
 |
|
Eighth step - integrating
the discussion to completion
Many discussions between doctor
and patient are only a torso; there is no "constructive beginning", the
thread of the conversation is not adhered to, and a clear summary is missing.
Proceed systematically. Take into account that every conversation has its
own "previous history", and should come up to mutual expectations. With
few exceptions, every conversation should include the following phases:
opening - adaptation - examination of the subject matter - closing.
The various phases in the
conversation are associated with different degrees of difficulty, and require
different questioning techniques. The most difficult phase is opening
the discussion. It is usually the stepping stone for all the subsequent
discussion. Remember Goethe's maxim: "He who misses the first button hole,
does not complete the buttoning". Ascertain at the beginning of the conversation
where your patient stands, and start from where he is, not from
where you are yourself. Go to where he is. Make use of the technique of
"funneling" as a principle for steering the conversation; use open questions
and widen the room for disclosure (open question technique), followed by
narrowing the field in which answers can be given in order to focus the
subject of discussion. Manage your discussions in the person-to-person
situation. Remember that successful dialogue is only possible if patient
is able and prepared to speak, and he is not inhibited or distracted
by the environment. Its success also depends on whether or not it is possible
to lead the interaction optimally by a combination of questioning,
listening and intervening whilst concurrently correctly interpreting
the verbal and non-verbal messages of the patient. Recognize when anxieties
are affecting the patient. Do not forget that it is easier to diagnose
than to interpret a disease.
Do not neglect that part
of the discussion which is the most important in other professional discussions
(selling a car or request of a loan), namely closing the discussion.
This has several functions: what has been achieved and what not?
What is now the position of the patient? Did the conversation fit mutual
realities? Taking stock of the discussion is a basic requirement for the
constructive
plan, i.e. prescriptions, advice, recommendations, suggestions as to
how these can be achieved and finally (if necessary) fixing a time for
another discussion. A satisfactory discussion is formal and structured,
with content and subject kept within bounds.
| top |
 |
|
Ninth step - establishing
a mutual (common) reality
The last step on the path of
perceptive discussion is the most difficult. It involves basic rethinking
in two particular regards: in one instance, despite often deeply ingrained
preconceptions, radically changing your thinking about reality.
Rethinking is also required because your approach to the patient will become
completely changed by this new apprehension of reality. This last
step, which is to communicate with the patient from a fresh understanding
of reality, is the most decisive step in understanding discussion.
If this does not happen, the doctor is completely prevented from entering
the world of his patient.
The initial condition
for the achievement of this last step is to jettison the ballast of the
old familiar preconception that there is only one single reality;
a fallacy that Watzlawick calls "the most dangerous of all self-deceptions".
Only when you have understood that there is "no absolute reality" in discussion,
but only subjective views of reality (which can be completely opposed
to one another), can one be released from the assumption that one's own
subjective reality is "true" reality. You must also become acquainted with
the fact that there are various degrees of reality.
The first degree is
based on the consensus of opinion of those involved, and on experimentally
repeatable and thereby verifiable evidence. One's own (that is, subjective)
reality is in fact reality of the second order. The implication
of this is that for one and the same thing, there are very many second
order realities, which are seen as "real" by those involved. As the second
order is as convincingly "real" as the first, there is a great danger that
the difference will be completely overlooked and we remain completely unconscious
that there are two different degrees of reality. It is impossible
to understand a patient unless we are prepared to accept the idea that
the reality of the disease to him is probably a completely different reality
to that which we perceive, and that each of these two subjective realities
(that of the doctor and that of the patient) are equally "real".
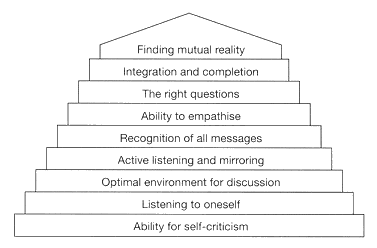
The nine steps to successful
conversation between doctor and patient
When you have accepted this
concept, you have overcome the most decisive obstacle of all. There is
no longer the danger that you will conduct your discussions with your patient
as if you were two players in a board game, unable to play a game together
because one was playing according to the rules of chess and the other to
those of backgammon. As long as both players are unable to find a mutual
code so that they can both use the same rules (that is to find a common
reality), it will be impossible for them to agree.
After this conceptual hurdle
has been overcome, you will be sure that the problem of communication is
nothing other than a search for common rules of play or mutual codes. As
long as each is an "outsider" to the reality of the other, communication
is not possible. Communication is the joining of two separate realities
by constructing a common reality.
Accepting that the reality
of your patient and your own are different, the next step is clear; you
must discover the patient's reality; where he is coming from, where
he is now, what moves him, what he would like, and everything from his
point of view. Empathy is the key to your approach.
Once you have understood
your patient's reality, the final step is to build a common reality together
with him. The identical reality of patient and doctor now opens
up the possibility of communication with a common frame of reference, and
each comprehending the other. When this is accomplished, doctor and patient
will have achieved the highest point possible in their dialogue.
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp33_steps.html
|
|