| So the patient dies,
in the typical style of our times, in the midst of the hectic activity
of a |
| supertechnicalized
and overmedicationalized medicine, in sterile rooms protected from the
dirty |
| world outside, after
many days of doctors battling to prevent his death. Cut off from all |
| communication with his
relatives, friends, colleagues and spiritual support, death now becomes |
| agony for the soul. Here
intensive medicine is the hell of loneliness, with the soul poised on the |
| edge of oblivion, in
the scientific research center within which the patient is totally lost
when he |
| grapples to come to terms
with the reason for his death, and the completion or closing of his life. |
| Heiner Geissler |
| Former Minister
of Health, W. Germany |
| Doctors should not force
people to die more than once. |
|
Prof. Burnet,
Nobel prize-winner, Medicine
|
| The impartial observer
will quickly become aware that all of the difficulties of medicine culminate
in |
| the intensive ward. |
|
R. Flöhl,
Journalist
|
| 1. |
Problems
with communication |
| 2. |
Exhaustion, disorientation
and false perceptions |
| 3. |
Anxiety, panic
and worries. |
Loss of communication
and lack of information create the heaviest burden for the patient
on the intensive ward. This has been shown in particular detail in the
"Vienna Model" (H. Thoma et al.). The quality of intensive medicine
depends to a great extent on the quality of communication between
those affected and those involved: the patients, doctors, nursing staff
and relatives. Each of these groups experience and judge intensive medicine
from completely different perspectives, or more accurately, from various
realities. There is no other branch of medicine in which the phenomenon
of differing realities has such an enormous importance as that within
intensive medicine, and nowhere else are the results of not taking this
phenomenon into account or ignoring it so grave. Only unbiased, open communication,
which acknowledges the perspective of the other, offers the possibility
of correcting or changing the public perception of the intensive medicine
over the long-term. The media still predominantly propagate the impression
of the intensive ward using terms such as "Death station", "Torture chamber",
"gloomy imprisonment", "inhumane medicine" or "sacrificial death" (see
also Heiner Geissler  ). ).
Intrinsically, intensive
medicine is neither humane or inhumane, in the same way that electricity
can be used for heating a house as well as for the electric chair. What
is decisive is that "intensive" medicine does not lose its own expectations
and objectives, which are those of making humanity more apparent in times
of extreme life-threatening conditions by offering appropriate medical,
nursing, technical, pharmaceutical and other resources for those whose
lives are in great danger (B.F. Klapp).
Communication is the decisive
factor which guarantees truly "humane" medicine (which is centered around
the patient), rather than the extensive use of all medical and technical
possibilities. Klapp puts this objective into a nutshell: "It is only the
relationship between people involved in events on the intensive ward which
will ensure that technology does not take on a life of its own, leading
both patients and staff to dread the impact that could be made by the machines.
Communication alone can prevent intensive medicine becoming apparatus medicine."
He looks at the present position of intensive medicine where he recognizes
"only a particular expression of our social relationships and their dynamics".
He projects this into the future, drawing the shocking picture of a society,
whose overriding motto is: "Try to do as much as possible for everybody",
in which intensive medicine could take on the ghastly role of the "final
obligation of the person to consume all that he can when terminally and
seriously ill".
Successful communication
in the widest meaning of the word can only be achieved in the area of intensive
medicine, where staff regard their work realistically and ultimately
based on a positive situation. It is stressful, often depressing
and occasionally exhausting to the staff that 20-30% of patients taken
onto the intensive ward will die there. However when these figures are
seen in another light, they become acceptable as well as encouraging and
motivating: 70-80% of desperately ill patients can survive or be saved
by the maximal involvement of human and technical resources.
An old proverb from China
can be used to guide the involvement of the doctors (which in the widest
meaning means not to act, but also to leave alone): "Treatment should not
be worse than the disease."
| top |
 |
|
The 4 realities
A patient who was treated
for some time in an intensive ward in Muenster after a serious operation,
wrote in her report of the experience: "I felt very safe and supported,
knowing that everything possible from a human point of view was being done
for my sake." She also wrote about the nightmares: "I dreamt, for example,
that I was in a laboratory, in which animal experiments were being carried
out. The infusion stands took on the appearance of gorillas, and X-ray
machines became dinosaurs."
A nurse who had been
working on the same intensive ward for 3 years reported: "I have certainly
learnt how to help the seriously ill patient with modern methods. Nevertheless
my feelings of helplessness and impotency are still there. These come up
especially when children die after a serious head injury, or when we cannot
save patients even after long periods of care and extensive treatment.
... I used to be woken by nightmares."
Twenty six out of 29 relatives
of patients who were asked for their first impressions of the intensive
ward in a study of the Aachen Technical University, chose terms such as
"horrifying, terrible, ghastly."
A doctor who had been
on a burns unit for a long period demonstrated to me with great precision
which sorts of German cars were particularly likely to be involved in accidents
leading to severe burns. When I asked if his job was depressing due to
the particularly unfavourable prognosis of extensive burns, he denied it
and said in fact they could produce very interesting pathophysiological
pictures.
These four descriptions from
patients, staff, relatives and doctors show how very differently reality
can be experienced in an intensive ward. The success of every communication
in the area of intensive medicine stands or falls on recognition of this
fact. If it is missing, even words can be deadly. Müller, Thywissen
and Behrendt (quoted in Hannich et al.) describe what was said to the relatives
of a 27-year old motor cyclist with severe brain trauma just before his
operation. The family were sent home by the surgeon with the words: "Don't
hold out too much hope, go home and sleep it off; we must all die sooner
or later."
| top |
 |
|
The patient's reality
Systematic studies of what the
patients experience, feel, expect and suffer have been initiated in the
last few years, and have shown more clearly which questions and anxieties
concern them. These studies have revealed that the patients themselves
do not always experience the intensive ward as an apocalyptic torture chamber.
Most studies from the various
areas of intensive medicine have shown that the majority of the patients
have a positive attitude to the time that they are treated intensively.
This is emphasized by Lawin: "Intensive treatment is judged much more positively
by patients than those who are not involved." The University of Muenster
(anesthetics and operative intensive medicine) found that 96.4% of patients
treated long-term thought that their treatment on the intensive ward had
been positive.
An example of how differently
patients and staff judged treatment on the intensive ward is shown in a
study from Unger and Bertel. 63 patients under 75 years old who were treated
on an intensive ward for acute myocardial infarction were asked about their
experience by means of a questionnaire. Staff were asked at the same time
how they would estimate the care from the patient's viewpoint. Whilst the
patients experienced admission onto the intensive ward, the initial therapeutic
procedures and the observation of machines as reassuring rather than producing
anxiety, the staff considered that this would be stressful. However what
the patients found negative and particularly difficult to bear, namely
the inability to determine the actual extent of their danger, did not appear
to the staff to be a problem of particular importance.
A group of Austrian anesthetists
and intensive care doctors developed the "Vienna model" for the psychological
care of seriously ill patients (G. Pauser). They randomly asked 50 patients
on discharge from three intensive wards to sort 52 statements into four
categories, in order to determine which factors result in the most stress
for the patient in the intensive ward. The conclusion was that the most
stressful items could all be included under the headings lack of information
and lack of communication. These were as follows:
"That I don't know how long
I must stay in hospital."
"That I only received superficial
information about my state of health and my illness."
"That I had such little
and such short contact with the doctors."
"That nobody told me what
the doctors had decided to do with me next."
The most important conclusions
of these results is that they not only find the lack of information and
communication as highly stressful factors, but at the same time show how
simple
steps could lower this stress.
Reports of the experience
of doctors who themselves were patients on intensive wards are illuminating
in two senses, as they are rooted in "two realities" (one of patient, and
one of doctor), and also because the descriptive problems of lay people
are not present. A professor of internal medicine who spent many days on
the intensive ward of a surgical clinic, wrote in his "Experiences as a
patient on an intensive ward": "I found it wonderful that the experienced
team, assisted by the watchful machines, would do everything to help me
overcome my serious illness and the subsequent operation. I noticed that
pain and restlessness were always alleviated, in as far as this was possible
without danger. Even now, I still feel deeply indebted to the staff and
doctors on the intensive ward." Here again the dominant feelings are those
of security and of thankfulness. The report is however critical of typical
stressful factors: "... the excessively loud noise on the intensive ward
created by speaking too loudly, doors slamming, the clatter of wooden heels,
the excessive use of glaring lights, the unalleviated monotony, the grid
on the ceiling which becomes a fixation point for anyone lying on their
back, the feeling of loneliness, occasionally accentuated by coolness of
the team."
A general practitioner (F.
Radermacher), who was admitted to an intensive ward with a severe heart
attack, describes how he too at first felt that he was in "safe hands".
As he asked the young doctor reading his ECG what he had, the doctor replied
"an extensive recent anterior wall infarct". Ventricular tachycardia started
a few seconds after receiving this information, and he had to be resuscitated.
After a bypass operation, this doctor also experienced severe pulmonary
oedema, which required intubation, tracheobronchial suction and artificial
respiration. Although intubation and tracheo-bronchial suction whilst conscious
are thought to be the most torturing procedures carried out in intensive
medicine, the doctor experienced this completely differently: "I felt as
though I was in heaven after suction and artificial respiration; as a result
of it, I had lost the unsupportable respiratory distress which I had suffered
with the pulmonary oedema."
Independent of the predominant
feeling of being helped that many patients experience, there are basic
situational stresses which can lead to frayed nerves over a period
of time (Wendt, as quoted by Hannich) (table).
| Most
stressful factors on an intensive ward from the patient's point of view
(M.
Wendt) |
| Lack
of assistance for orientation |
| Missing diurnal-nocturnal
rhythm |
| Sensory monotony
(constant rhythmical noise) |
| Sensory hyperstimulation |
| Chronic lack
of sleep |
| Excessive illumination |
| Lack of communication |
| Separation from
friends and relatives |
|
The difficulties which arise
in trying to maintain a continuous relationship with the treatment team
have been quantified by film analysis. Wendt photographed 6 patients every
15 seconds over a total of 290 hours. On average something changed in the
area of the patient every 104 seconds. On average 1-3 minutes were spent
with the staff). This means that the patient has neither peace nor meaningful
contact. Sych (ref. Hannich) found that "wish and complaint books" revealed
that patients were particularly upset by too little personal contact with
doctors, insufficient answers to their questions during ward rounds, and
the uncertainty which arose after catching fragments of conversation.
The much publicized threatening
nature of the "apparatus medicine", which is supposed to be
extreme in intensive medicine, is probably far more likely to exist in
the realities of relatives, the media and also the staff of the ward, than
in the reality of the patient himself. Many patients report that they were
not upset, and often not in the least afraid of the apparatus (monitors,
respirators, infusion pumps etc.). The technical intervention was mostly
not seen as threatening, but rather experienced as an element of security.
G. Hensel who was a patient on an intensive ward writes: "The patient feels
that he is supported, and his worth great when he recognizes that he is
surrounded by such an extreme investment in technology. He immediately
sees how expensive everything is. It reassures him to know that such a
large amount of money has been made available for him, and does not raise
anxieties. It is not the machines which shock him, but (occasionally) the
people who use them." Anxiety can arise quickly if the patient senses that
the staff are not fully conversant with the apparatus. The feeling of security
is rapidly converted to insecurity and to feelings of exposure.
The effect of treatment
in an intensive ward very much depends on the situation leading
up to admission. Patients with chronic prior illness (e.g. chronic
respiratory insufficiency) view the decompensation of their illness as
insoluble and hopeless. If a spell in the intensive ward succeeds in recompensing
them, this can also have a positive reaction summed up as: "I will make
it this time as well."
Patients who are admitted
to the intensive wards neither expecting to be admitted, or prepared
in any way (after infarction, accident or postoperative complications)
also do not initially experience any serious problems of adaptation. This
type of reaction can be seen particularly well in coronary patients, who
are often unconsciously regarded as "favorite patients" by the staff, as
the majority stabilize within two or three days and can be transferred
to the general medical ward. This initial "neutral" reaction to the intensive
ward and the positive opinion are however limited: if a longer period is
required for intensive therapy, the amount of criticism of the intensive
ward gradually rises (from the third or fourth day).
In patients in whom the admission
is planned (after major operations) a positive attitude is predominant,
and the intensive care is well tolerated as an additional measure which
reassures. This is however a rather different situation in that the aspect
of intensive observation is more important than that of the intensive
therapy.
In all cases, the patient
experiences his situation as exceptional. "What does this extraordinary
condition feel like? Whoever is admitted to an intensive care ward is there
because of a life or death situation, regardless of what his chances are.
... Nobody on the intensive ward can ignore the fact that life is not a
gift but rather a loan: that one (on this earth) cannot own anything; that
he can only use it for a limited period. The patient has to come to terms
with the thought that his period of loan can expire. For the first time,
death is for him not simply a distant but a very close eventuality, perhaps
even inevitable. He can no longer think without considering his own death
... In this extraordinary situation, nothing is as important as himself.
Therefore one should not judge the enormous selfishness of the patient,
but rather try to understand it. It belongs to the self-healing powers
of the patient; it is an egoism hallowed by the will to live. It is part
of the extraordinary situation that the patient feels his soul to be very
seriously wounded." (G. Hensel, a former patient).
Klapp describes this disturbance
of the self-worth as follows: "The most important factor is that of
limitation of the ego functions (in the psychoanalytical sense of the term),
which the patient experiences with pain, and which can make him very anxious.
This anxiety can be understood as that before annihilation (and should
not be confused with fear of death)."
The very real dependence
in which the patient finds himself is experienced differently depending
on the severity of the illness and the particular phase in its progress
and has to be taken into account in the treatment plan. The degree to which
the patient reacts to the disturbance of feeling of self-worth plays a
very important part in the extent to which the patient "can allow himself
to surrender, relax and regress, right back to the level which closely
resembles the early childhood dependence situation, and then as clinical
improvement occurs, to gradually progress from reliance on others to rehabilitation".
| top |
 |
|
My heart stopped
A 53-year old general practitioner
describes his experiences as a patient on a coronary care unit.
| "The publisher of this book,
who is also a friend, asked me to share my memories of an intensive ward.
I did not agree initially. As time went on, and I had time to think over
what had happened during my illness, the easier it became to decide to
write this report, simply to remove fear of the intensive ward from anyone
who reads this book. I know that these units arouse anxiety, uncertainty
and perhaps doubts in many people, including doctors.
After Christmas dinner in
1984, I suddenly experienced very severe pain in the cardiac area, with
sweating and dizziness. The pain became worse and worse, and I became immensely
anxious. I went to a mirror and realized that I was as white as a sheet,
with beads of sweat on my brow, and I knew exactly what had happened -
heart attack. However I did not want to believe it. I did not want to accept
this could happen to me.
In the emergency department
of the hospital, the duty doctor read the ECG and mentioned briefly and
crisply that there was an extensive anterior wall infarction. I understood,
and immediately lost consciousness. I was unconscious on the coronary care
ward for 10 days. I was resuscitated and defibrillated several times.
I must mention that had the
diagnosis been given without the 'full truth', it is possible that my shock,
which could have been precipitated by it, would not have been so extreme.
I myself have often been called to heart infarctions. All my patients survived
up to hospital admission, as (as well as treating them medically) I also
took great care to alleviate their psychological condition. I comforted
them, and assured them that it was not as bad as they might imagine, and
avoided directly answering the blunt question: 'Is it a heart attack?'.
Everybody knows what infarction means and the dangerous situation it imports.
After I had come out of the
very deepest level of unconsciousness, I found myself in a twilight state
in which I had no idea where I was. I was not fully orientated, and thought
that I was on an island, but was aware of my family visiting me on the
unit. I can remember more clearly the transitional syndrome which I experienced;
I accused my colleague of treating me incorrectly. I would not prosecute
directly but would ask a mutually-known solicitor to determine the legal
situation. Thank God, this transitional state did not last very long. I
slowly became fully orientated, aware of my situation and surroundings,
and was able to observe what was going on.
With time, I got to know
many young, very concerned colleagues and lovely, kind staff on the intensive
ward. I noticed that nurses and staff are all well-trained and idealistic
young people. They work round the clock, know just what to do, are always
ready to help, and are patient with and observant of those in their care.
They suffer with the severely-ill patients that they look after. They are
the first to be confronted with a deterioration of the patients. They know
this, and often feel overwhelmed.
Many people prayed for me
at this time and I am convinced that this helped me. I would like to refer
to the randomized double-blind trial carried out by Prof. Randy Byrd of
the University of California (see chapter on talking about God  ). ).
Outsiders and also the media
falsely judge the worth of the coronary care unit, with its highly technical
equipment. I was very reassured by the intensive ward, both as a patient
and as a doctor, as I knew I was under constant supervision, and that everything
was there should there be a change in my condition. The apparatus had a
very calming effect on me, and certainly did not make me anxious. I found
minor things much more stressful, such as using a bed-pan, the bladder
catheter, and prolonged infusion.
It was not only sterile and
business-like on the coronary care unit. There were jokes and laughter.
I met many people on my long journey on the intensive care unit, most of
whom impressed me, because they were idealistic, open, and busy. Intensive
ward sisters and staff told me that the responsibility was enormous and
hardly bearable, and that they felt not only physically but also psychologically
drained by this prolonged lack of personnel in the intensive care unit.
They felt that they would lose too much of themselves if they were to work
more than two or three years on such a unit.
On the second day after my
coronary bypass operation, I developed severe pulmonary oedema, which resulted
in the need for a further two days of intubation. I myself experienced
what lung oedema really feels like. This tantalizing need for air, this
lack of oxygen, gives rise to acute feelings of suffocation and constriction.
I lost consciousness during
the reintubation, but as I came round I could breathe well with the help
of the respirator and received fresh air. I felt as though I was in seventh
heaven, and was so thrilled to have air once again. As I was unable to
communicate by voice, I had to write my requirements on a board.
Why then have I written this?
Very simply, to make the situation of an intensive ward known to my colleagues
and the lay public, and to remove anxiety from the situation, whilst at
the same time to make it know what a blessed place it can be. Intensive
units certainly give immense help, and everyone should know that many idealistic
people work on them." |
|
| top |
 |
|
Doctor and staff
(the treatment team)
The patient's "reality" and
that of the team are usually discussed from a theoretical point of view.
In fact the two realities should not be considered separately. There is
a great danger in not taking into account the almost incomprehensible relationship
which they have to one another. Klapp has been particularly concerned with
the structure of the relationship between patient and treatment team, not
only in theory but also practically in clinical settings, and emphasizes
this point as follows: "This teaches that the patient can but artificially
be considered alone, since he is always dependent on the context of therapy.
This also applies to the second group in the relationship; that of the
treatment team."
It is obvious that intensive
medicine is viewed very differently by the doctors and by
the nursing staff. This is due to the fact that each group attending
the patient has different areas of competence, different responsibilities
and different resources at their disposal.
Generally the doctor
is involved at a higher level of activity, and he is required, and often
forced, to take decisions with far-reaching consequences. His communication
with the patient is concerned more with information rather than relationship,
contact with the patient is considerably shorter - he is more able than
nursing staff to escape from emotionally-charged situations. Probably he
is more likely to experience success and less likely to feel guilty. On
the other hand, the daily tasks of the nursing staff mean that they
are more deeply involved because of the continuous contact with seriously
ill and dying patients. This frequently results in "feelings of failure,
disappointment, grief, guilt, but also anger" (B.F. Klapp).
| Major
stress factors for a treatment team on the intensive ward |
| 1. |
High
physical and intellectual stress |
| 2. |
Problems of communications |
| 3. |
Conflict situations
(patient, team, relatives) |
| 4. |
Time pressure |
| 5. |
Anxieties (one's
own and those of others) |
| 6. |
Disappointment |
| 7. |
Feelings of failure
and of guilt |
| 8. |
Confrontation
with one's own mortality |
|
Both groups carry out their
work in a climate of highly tense expectation and maximum responsibility,
along with particular competence and increased readiness to be involved.
It is very rare to find somebody who is "used" to the extreme situations
of intensive medicine, even after working within it for many years. It
is an illusion to believe that one can maintain professional "affective
neutrality" after working in an intensive ward for any period of time.
More often defense strategies develop, which make it possible to
carry on under such enormous stress. This stressful situation with the
character of dilemma particularly affects the nursing staff who find
themselves in this "chronic situation". The dilemma is that if the treatment
on the intensive ward is successful and the patient returned to a normal
ward, the nursing staff apparently have this success snatched from them,
as the patient is lost to them. If the patient dies, his death is experienced
as a blow and feelings of guilt arise.
There are a series of defense
mechanisms which the treatment team can develop, which may of course
distort the relationship with the patient.
| |
"Avoiding"
the patient, with an increased interest in the apparatus |
| |
"Denial"
on the affective level, which results in over-playing of the stressful
situations by sternness (quoting rules), distancing, cool tone of voice
or displaced humor |
| |
Activism
leading into depressive or grieving moods and the associated emotional
withdrawal |
| |
Blame-shifting,
which can be expressed for example by the fact that sisters do not report
death (which is constantly present) as the largest single stress factor,
but rather "difficulties in lifting patients" (B.F. Klapp) |
The structure of the relationship
between the patient and the groups of helpers is determined
by two elements, one of which is asymmetry and the other polarity between
active and passive.
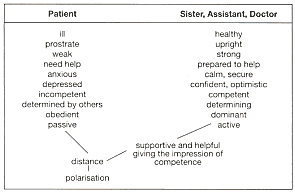
Dimensions in the relationship
of the patient to the treatment team. Differences between the relationship
of the therapy and roles (expectations) (B.F. Klapp)
The following types of relationships
between patient and the treatment team appear fairly frequently and their
recognition is helpful in the resolution of conflict between the two (Klapp):
| 1. |
The
patient
experiences the distance (see figure) between him and the team to an
extent which is supportable. It is thereby possible to accept the treatment
team allowing hope, surrender and the necessary regression to develop naturally. |
| 2. |
The patient
experiences the relationship with the treatment team with severe polarization.
Feelings of being threatened result from this, followed by severe anxiety,
associated with deep suspicion and a desperate attempt to maintain a sort
of pseudo-autonomy. Such patients are seen as "difficult" in view of their
inconsiderateness, their tightly-controlled behaviour and their know-all
manner. If the team respond to this type of reaction with excessive dominance,
insistence, competence and positional strength, the situation cumulates
in a sort of vicious circle (see chapter on the "difficult patient"  ). ). |
| 3. |
The problems
with another group of patients result from their difficulties in accepting
their illness. These patients repress their anxieties and depression,
continue to behave as before and appear calm. They fit into the situation
in the intensive ward and act particularly appropriately. Many patients
with cardiac infarction belong to this group. These patients are often
regarded as "ideal patients" by the treatment team. |
| 4. |
A further very
critical type of response can develop when the patient regresses.
These patients tend to show obvious infantile behaviour, they are overwhelmed
by anxiety and feel completely dependent on the treatment team. They land
up in a situation which is characterized by hopelessness, associated with
severe anxiety, later denying signs of improvement and refusing to leave
the intensive treatment. If the treatment team react to this with increased
concern and excessive activity, anxiety becomes even more marked. The increased
clinging behaviour of the patient can finally lead to rejection by the
team. |
The recognition of these
types of reactions, their roots and effects, is the key to relationships
within the team which avoid counter-transference of anxiety, emotion and
thoughts.
It underlines the importance
of communication within the treatment team. Klapp says, "the potential
for empathy increases to the extent that the treatment team can expose
and come to terms with their own weaknesses, anxieties, uncertainties,
and admit their own needs for care. Thus, they can deal with the patient
more flexibly and can modify rigid defense strategies and the pattern of
relationship resulting from them."
The way in which a patient
manages anxiety and stress which he experiences on the intensive ward,
is to a large extent dependent on the behaviour and approach of the treatment
team.
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp26_intensive_medicine.html
|
|