|
Discussion with the suicidal patient
The approach to the suicidal
patient is not the exclusive domain of psychiatry. The general practitioner
experiences the suicidal patient in the presuicidal phase and the physician
in hospital usually meets him after a suicide attempt. A Swiss study showed
that
92% of those with "suicide attempts" and 86% of those with "successful
suicides" had been treated by one or more doctors in the preceding six
months, and about half of them had been regular attendees. The majority
of patients (76% of those attempting suicide and 58% of those who committed
suicide) had been treated by their general practitioner. The doctor and
patients had usually known each other for many years, but nevertheless
more than a third of the doctors were "shocked" to hear of the suicide
or attempted suicide.
About 250000 patients per
year are seen in West Germany for inpatient treatment following suicidal
actions. 14000 kill themselves, and it is estimated that this includes
about 3000 patients with endogenous depression. 16% of those who survive
their attempt at suicide, repeat this attempt in the following year. The
likelihood of a repeated attempt is highest in the first year after the
initial attempt. At least 85% of those attempting suicide could be released
from intensive care within a very short time. 15% had to be admitted to
a psychiatric ward or hospital due to further suicide attempts or endogenous
depression (H.L. Wedler, M. Philipp, H.J. Bochnik).
Doctors and nurses regard
suicide patients as the "most disliked patients". As a result, there is
a great lack in the psychosocial care of suicidal patients. There are many
reasons for this negative opinion as regards the suicidal patient. It is
very often presumed that "he did not really mean it". It is usually only
those who undertook the more serious attempt who have a chance of being
taken seriously. The subjective side of the patient is completely dismissed
during the clinical separation of the "tried-on" suicide attempt on the
one hand and the "serious" attempt on the other. Many doctors find it very
difficult to accept the attempt as a signal for help by which the
patient is indicating that he is at present unable to go on with the resources
at his disposal (C.H. Reimer).
There are several reasons
for this unsatisfactory care of the suicidal patient. The way of dealing
with the suicidal patient is rarely taught during the medical studies and
in the training of nursing staff. Psychosocial care of suicidal patients
is very often delegated to psychologists and to psychiatrists. This automatically
leads to an emotional withdrawal from the patient with the inevitable negative
effects on communication. Working with a suicidal patient raises a variety
of anxieties, aggression, stresses and conflicts, as well as personal
uncertainties about death. Problems raised by the frequent lack of compliance
add to this. Many patients refuse to discuss the attempted suicide and
demand immediate discharge. This raises the feeling in the helper that
he is being rejected.
There are two major areas
to consider when presented with a suicidal patient:
| 1. |
Recognition
and assessment of the likelihood of suicide. It is not possible
to prevent suicide unless this is appreciated. This particularly
difficult responsibility mostly falls to the doctor who is least trained
in this area (general practitioner). |
| 2. |
Care after
the attempt which is mainly in the hands of the hospital doctor. |
| top |
 |
|
Recognition and assessment
of the likelihood of suicide
H.J. Bochnik (University of
Frankfurt) believes that probably 7000 suicides could be prevented per
year in West Germany if there were fewer mistakes in the recognition and
the treatment of suicidal patients, especially those with depression.
Recognition of the likelihood
of suicide and the risk of suicide are one of the most important responsibilities
which the doctor can be faced with. They can create major problems even
for a doctor who has had a great deal of experience in the area. Testing
by psychological, psychiatric or psychosocial methods cannot be used to
assess the risk, as long as their reliability for prediction remains uncertain.
Here it will be attempted to show what possibilities there are for the
doctor who is not trained in psychology or psychiatry to use in his practice
to estimate suicidal potential. Except in panic actions, attempts at suicide
are, as a rule, preceded by a presuicidal development (W. Pöldinger).
This can be broken down into three stages (figure):
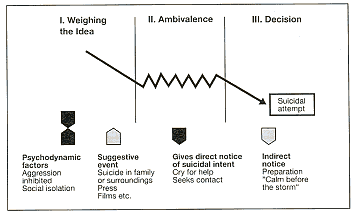
Stages in presuicidal
development (after W. Pöldinger)
Stage 1: idea of suicide
Stage 2: ambivalence
Stage 3: decision
In the first stage, suicide
is considered as a possible way of solving a problem or conflict.
There are psychodynamic factors such as aggression (which cannot be expressed
and are turned inwards) which play a role, but there also may have been
suggestive events (suicide in the environment). This explains the observation
that the reports of suicide of prominent people can raise the suicide rate
in the population. It was shown that the suicide rate fell markedly during
a newspaper strike in Boston.
In the ambivalent
stage, a battle develops between self-preserving and self-destructive forces.
Direct or indirect warnings of suicide can appear in this stage
(suggestions, threats, predictions), which are to be interpreted as cries
for help and attempts for contact. The presumption that "those who talk
about suicide don't do it, and those that do it, don't mention it" has
not been shown to be valid. About 80% of all those who attempt suicide
have given warnings of their intention. This is usually not taken seriously
in cases where the person in question thereby puts pressure upon others.
The decision either
for continuing life or for suicide is taken in the third stage. Those around
are aware that the person has become "calm" and no longer mentions suicide.
However it would be wrong to presume that there is no longer a risk of
suicide. It is much more likely to be the "calm before the storm". It is
particularly important to ask somebody who has mentioned or threatened
to commit suicide why he now wants to live. Those who truly want to live
will immediately be able to give a reason, whereas the person who has decided
to commit suicide is not able to find a satisfactory answer.
If there is any suggestion
that the patient is suicidal, even though he has not mentioned it (depression,
life crisis), it is better to speak to him directly and confront
him rather than fall into a false sense of security. This applies especially
to the general practitioner who has known his patient for many years, who
can be led astray by a false perception. Even though he has known the patient
for many years, he only knows a few sides of the person, and if suicide
is under consideration, this longstanding relationship is no substitute
for such a discussion.
When trying to assess the
suicidal
behaviour, it is very important to take into account the fact that
there are different psychodynamic's between suicide and attempted suicide.
In the case of suicide, self-aggression and self-destruction are
at the forefront. Although a suicide attempt can actually be a failed suicide,
it can also be parasuicidal behaviour (N. Kreitmann W. Feuerlein,
cit. W. Pöldinger). The parasuicidal gesture is not really an unsuccessful
attempt at suicide, but rather an attempted suicide in which a cry for
help is foremost. It is a form of non-verbal communication, which is
used because verbal communication is no longer possible. This is the explanation
of the fact that suicide attempts are observed more commonly in younger
people, and suicide itself is more common in
older people.
There is a rising number
of young people in West Germany who commit and attempt suicide.
Suicide is the second most common cause of death in those between 12 and
15. Suicide was the cause of death in 12% of those between 15 and 19 (1974
to 1983). Many patients committing suicide could not manage separation;
many school systems no longer maintain an intact class from the age of
15, and the pupils have hardly any contact with others as they dash from
one course to another. If there are family crises on top of this (such
as divorce of the parents), the loss of a reference person can lead the
young person to suicide.
The other group of those
particularly at risk of suicide are old people. Statistics show
that old people living on their own (widows or divorced) are particularly
at risk of suicide, especially when they are faced with the loss of a life-long
partner. Loneliness and isolation put the old person at much greater risk
of suicide. Old people who live in an old people's home can also feel lonely
and isolated, as it is not the number of social contacts but rather the
quality
of relationships which is decisive.
Doctors, too, are not immune
to suicide, as shown by their suicide rate which is even higher than in
the general population. This is probably a reason for inhibitions in speaking
to a patient at risk of suicide.
[IMAGE]
Distribution of suicide
and suicide attempts according to age (after Dotzauer, 1963)
W. Pöldinger lists 4
points which should be used in the assessment of the likelihood of suicide:
| 1. |
In
any group with raised risk factors |
| 2. |
Crises, changes
and pressures |
| 3. |
Suicidal development |
| 4. |
Pre-suicidal
syndrome |
The following groups are
at risk of suicide (Kiev and Wilkins):
| 1. |
Depressed
patients |
| 2. |
Alcoholics, and
those addicted to medication or drugs |
| 3. |
Old and lonely |
| 4. |
Those who have
made it known, by mentioning or threatening attempts on their life |
| 5. |
Those who have
already attempted suicide. |
A crisis is often a precursor
of the suicide. Crises are defined as stresses and experiences that the
affected person can no longer work through and overcome (Häfner, 1974).
Suicide is then one possible strategy available to solve the problem; acknowledgement
of this reaction to such a crisis gives the doctor a chance of recognizing
the risk of suicide. Nevertheless there are great individual variations.
Crises can be seen as "normal" life-changes (leaving home, marriage, retirement)
or as shaking experiences such as death of a loved-one, serious illness,
social rejection etc. The majority of crises are probably satisfactorily
resolved within the social circle. On the other hand, reactions to environmental
crises can persist and become chronic. One of the most significant reasons
for
suicide
however appears to be that those around do not react to a crisis.
The danger of the development
of a presuicidal syndrome arises if the crisis remains unresolved
(E. Ringel). This development occurs in three stages and offers an important
chance for the assessment of a suicide risk (Ringel, 1969).
| The
presuicidal syndrome (after Ringel, 1969) |
| 1. |
Increasing
withdrawal:
situational, dynamic and in interpersonal relationships and society. |
| 2. |
Storing up
of aggression with release against himself. |
| 3. |
Fantasias
about his own death by suicide (initially called up but imposing themselves
as time goes on). |
|
The inhibition and withdrawal,
especially that of affect, is relatively easy to recognize. It is much
more difficult to recognize aggression directed against the subject himself.
Suicidal thoughts and desire for death, especially when they impose themselves
upon the patient, take on a great significance. In order to make it easier
to recognize, W. Pöldinger has suggested a simple list of questions
for the suicidal patient (table).
| Questions
to determine a suicidal intent (W. Pöldinger, 1982) |
| Risk
of suicide |
Have you ever
thought about taking your own life? |
| Preparation |
How would you
do it? Have you already made preparations? (The more concrete ideas, the
higher the risk) |
| Tempting thoughts |
Do you mean to
think these thoughts or are you tempted against your will? (Spontaneous
thoughts are dangerous) |
| Giving notice |
Have you already
told somebody about your intention? (Always take warnings seriously) |
| Inhibition
of aggression |
Are you angry
with somebody and having to suppress this anger? (The aggression which
has to be suppressed turns against the person himself) |
| Withdrawal |
Have
you reduced your interests, have thoughts and social contacts been more
limited lately? |
|
Recognition of the likelihood
of suicide is the first step towards suicide prevention, and the
exposure of the reason (conflict situation, depression) is the next.
There is usually no difficulty
in recognizing marked depression: it can be generally described
as a ... lessness syndrome; uselessness, hopelessness, sleeplessness with
loss of motivation and trust.
It is more difficult to recognize
a masked depression, which by its very nature cannot be picked up
by complaints or their content. Hints may be gleaned from the absence of
an organic correlate to the complaint together with a dramatic description
of the symptoms (i.e. "as if a bowl of gall were tipped over my tongue...")
(P. Kielholz, 1973, L.S. Geisler, 1973).
Meerwein underlines that
the affective reaction of the doctor can also be indicative of hidden
depression. If the doctor becomes aware of a depressed feeling or mood
in himself whilst the patient is describing his symptoms or problems, he
should be aware that this may indicate depression in the patient.
If depression is likely to
be present, the treatment with appropriate antidepressives (not however
psychopharmaceuticals of the benzodiazepines groups) should be commenced
as soon as possible. The severity of the depression and the experience
of the doctor in dealing with depressed patients determine whether or not
a consultant psychiatrist should take over the case. Where there is the
slightest doubt, but especially where there is clear suicidal intent, psychiatric
therapy should be requested.
There is a series of general
rules for the medical dialogue with depressive patients. Tension
can be reduced by the doctor clearly indicating to the patient that he
understands
such depression. It is usually ineffective to attempt to "console"
the patient, as the depression itself is "hopeless" and the condition inconsolable.
It is equally ineffective to attempt to try to animate the patient by suggesting
obvious or superficial approaches ("completely relax at the weekend", "pull
yourself together as much as possible"). The depressed person is neither
able to completely relax nor to mobilize himself. "Pull yourself together"
is understood in the literal meaning of the phase, as the injunction only
increases the demands on him. Attempts at distraction (journeys, holidays,
and visits to cinema or theatres) are equally useless. Similarly, "patting
on the shoulder" is also likely to fail ("it will soon be better again"
etc). The determining factor is that the depressive feels that his symptoms
are accepted and understood. It can be a relief to the patient to hear
that it is known that depression can resolve as quickly as it comes on.
| top |
 |
|
Dialogue after a
suicide attempt
The care of the patient after
a suicide attempt usually takes place in a general hospital. In fact the
care is usually limited to the treatment of organic signs ("detoxification").
This therapy leaves the patient with his problems unresolved, as well as
with the additional burden of the stigma of the failed suicide attempt.
Even consultation with a psychiatrist really only has the function of sorting
out those patients with acute psychoses or psychiatric diseases which are
in urgent need of treatment. The majority of suicidal patients (90-95%)
remain unsatisfactorily cared for within this system. It is however possible
to achieve satisfactory care for these patients by the introduction of
a liaison psychiatrist, who advises the medical team concerned with
the patient, also involving social workers, psychologists and ministers
where necessary. As yet, the system of the liaison psychiatrist in only
found in closed psychiatric departments; it is very infrequent to find
the American concept of specialized crisis intervention available in Germany.
In other words, the care of the suicidal patient in the hospital does not
usually fall on specially trained doctors; however they have the following
important responsibilities (Goll and Sonneck, 1980):
| |
Building
up of a relationship: effective initial conversation, offering a listening
ear, understanding, readiness to help, reassurance, defusing of anxieties
and soothing. |
| |
Assessment
of the condition of the patient, the severity of the problem, and the
risk of suicide. |
| |
Recognition
of his own abilities and possibilities to deal with the situation,
with regard to passing the patient on to a more suitable organization (certainly
not
"sending away"!) |
| |
Construction
of a plan for help, along with the patient, which should be built up
of small steps so that the objectives of intervention can be achieved within
a short period. This help for self-help is suggested by various
methods. The patient must be released from emotional pressure by expressing
and discussing his anxieties, guilt, aggression and suicidal thoughts.
Distancing from the crisis situation can be achieved by looking back over
the precipitating factors as well as the associated feelings, perceptions
and possible consequences. The patient should be encouraged to use his
own initiative, and social reintegration should be achieved as soon as
possible. |
| |
A plan for behaviour
in the event of new reasons for crises should be worked out. |
Experience has shown that
the initial discussion after a suicide attempt takes on a decisive
role. Every single word and every reaction that the recovering patient
initially hears at the hospital bed can be decisive for the further course
of his life. This is because the suicide patient perceives these first
contacts as the reaction of the environment to his suicide attempt.
It is for this reason that further working out of the conflict and attitude
to his failed attempt at suicide depends on whether he receives friendly
acceptance and readiness to help or rejections, judgement and indirect
punishment. Hans Ludwig Wedler stated: "The type and quality of the first
verbal as well as the non-verbal communication at the hospital bed is most
likely to decide whether the patient once again accepts the reality from
which he tried to escape, as well as his willingness to accept further
help. A smile from the doctor and the nurse, a single friendly word are
in themselves already 'positive crisis intervention.'"
The objective of crisis
intervention after the suicide attempt is to create a correct approach
for the future. Wedler gives 7 steps in the approach to the suicidal patient
which act as crisis intervention.
| 1. |
| Contact as early as possible
(bearing in mind the importance of the initial conversation) |
| Message: "I am prepared
to accept you." |
|
| 2. |
| Opportunity for
self-examination |
| Message: "I am prepared
to listen to you." |
|
| 3. |
| Re-establish social relationships
(to nursing staff, doctors, other patients); |
| Message: "Neutral atmosphere
for practicing social contacts." |
|
| 4. |
One-to-one discussions,
with analysis of the psychosocial situation and the way in which
the crisis arose; discussions with close relatives; family and spouse
discussions. |
| 5. |
Pointing in
the right direction for further therapy and follow-up; motivation of
the patient; arranging introductions. |
| 6. |
Attempt to integrate
the suicidal behaviour into the psychosocial relationships of the patient
(metacommunication). |
| 7. |
Putting the
personal helping role into context. |
It is not possible to achieve
this form of crisis intervention without a considerable expenditure of
time. Wedler estimated that a complete crisis intervention takes on average
5 to 6 one-to-one discussions and 1 or 2 discussions with relatives.
There are two psychological
factors which can limit the effectiveness of crisis intervention (M.
Philipp):
The majority of suicidal
patients that survive the acute or intensive care ward have a transitional
syndrome which lasts several hours or days after the phase of detoxification.
This transitional phase is usually limited, and consists of slight attention
disturbances and affective lability. This means that discussions, advice
and suggestions are very often forgotten in the detoxification phase due
to this amnesic component. This underlines the importance of several
discussions.
A further psychological barrier
in the intensive care unit is the tendency of repression and denial
on the part of the suicidal patient. This mostly has its roots in a premorbid
disturbed development of self-worth. This expresses itself as an excessive
ego ideal and a increased tendency to feel injured. The failed suicide
attempt along with surrendering to the intensive care unit act to increase
damage to the ego which he attempts to resolve by means of repression and
denial. This is also the reason why earlier suicide attempts are played
down (also by relatives). This behaviour pattern is seen for example in
the strong pressure for early discharge and refusal of psychological or
psychiatric care.
In leading a discussion
with suicidal patients, it is particularly important to avoid all disparaging
comments and critical remarks about suicide. The importance of this must
also be impressed upon the relatives. The objective of discussion
with the suicidal patient is to build up a feeling of self-worth, and not
only to work out the problems surrounding the patient. This can best be
achieved by a basic approach, which accepts the patient without prejudice
and gives him the feeling, by the way in which he is treated, that he is
understood. "Taking the subjective experiences of the suicidal patient
seriously is more helpful than lengthy discussions about the suicide intent
and trivializing the problems" according to M. Philipp.
Most life crises run through
the phases of shock, reaction, working out and new direction
(Cullberg, 1978). The suicidal patient is in the shocked phase. The essence
of every care of suicidal patients therefore can be summed up by the formula:
"Depending on the phase of the crisis ... a personal presence is in the
forefront at the time of shock, the 'just being there' and 'standing by'
(the 'representation of hope')" (G. Sonneck).
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp25_suicidal.html
|
|