| Medical ethics, more than ever
before, need |
| to proclaim that health
is not the absence of |
| impediments, but rather the power
to live |
| with them. |
| Dieter Rössler, physician
and theologian |
Raspe defined chronic illness
as follows: "We refer to illness as chronic, if it creates hardship for
the body or mind of the patient (and usually for others) for the rest of
his life." These impediments can be specific to the illness, such as chronic
shortness of breath in asthmatics, difficulties in getting about in rheumatoid
arthritis, but can also be common to all chronic illnesses: the need for
continuous therapy and follow-up, social isolation, uncertainly about the
future, unemployment or lost career opportunities, difficulties with those
around them, as well as stress caused by lack of explanation.
| top |
 |
|
Acute and chronic
illness
Acute and chronic illnesses
are completely different forms of being ill. Recognition of this
difference is a prerequisite for an appropriate medical approach and behaviour.
It also involves the doctor accepting that he is involved in the
care of the chronic sick. Hartmann puts it succinctly: "For the patient
who is chronically sick, his doctor is 'chronically Doctor'". He goes on:
"What this implies is experienced by every doctor who has cared for a chronically
sick patient over 10 or 15 years. When this patient dies, the doctor notices
it and is aware of how this patient had become part of his own identity.
He grieves for him, and this grieving is, as with close relatives, a restoration
of his lost identity."
| top |
 |
|
From the viewpoint
of the patient
Chronic illness is characterized
by the following (Schmidt, Hartmann):
| 1. |
Prolonged
illness of unforeseeable duration. It is important to recognize that a
large proportion of "highly informed chronically ill patients" cherish
concrete hopes for an end to their illness. Hartmann estimates this to
be 50% of all those with chronic rheumatoid disease. |
| 2. |
Long-term
concerns and stress, often associated with a latent dread of death. |
| 3. |
Knowledge
of the incurability, with at most a chance of being able to manage
in spite of irreparable impediments. |
| 4. |
Long-term
damage, left in the wake of the disease, which prevents success
in certain careers or limits personal development. |
| 5. |
Continual
need for check-ups, observation, treatment and/or nursing care i.e.
the continual dependence on others or on apparatus and machines
(dialysis patients). |
| top |
 |
|
Learning to cope
with chronic illness
It is almost impossible to be
ill for a prolonged period without going through a process of coming to
terms with it. Although the individual repertoire of coping strategies
show a great variability, there are a series of basic mechanisms of a general
sort, which can be grouped together under the heading effacing up to
it. Knowing about them is of great importance in the care of the chronically
sick. There are two important reaction patterns:
| |
Defense
mechanisms |
| |
Coping behaviour |
Defense mechanisms are
processes of working through the situation, which usually are unconscious,
caricature reality and have the objective of temporarily dealing with threats
and anxiety. Direct evidence of them disappears if this mechanism succeeds
and only indirect effects hint that defense mechanisms have been effective.
An example is seen in a patient who exhibits marked discrepancy between
his balanced or even euphoric mood and the severity or hopelessness of
the illness.
One of the most important
defense mechanisms is that of suppression. In this way, "motives,
moods and ideas that the ego can not manage are not taken into consciousness
or are split off, mostly in an unconscious process" (Schmidt). The patient
no longer needs to try to cope with reality, and moves around in a more
healthy world that he has constructed for himself. The most extreme form
of suppression is denial which can be seen often in cancer patients.
However this process of denial cannot be maintained continually and completely,
so that the observer may see confusing swings between "knowing and not
knowing".
A second important defense
mechanism is regression. This is understood to be "the replacement
of complex forms of satisfaction by one or several, perhaps even all, motives
in the person by more primitive forms of satisfaction. Put in another way,
regression is the recourse to primitive (earlier) levels of motivational
development" (Toman, 1978). These can be seen particularly clearly in some
patients during prolonged periods in hospital. These patients act childishly,
becoming dependent and limited. Eating, drinking and bowel action become
dominant in their lives. The "career patient" can be understood as an extreme
example of regression. The patient plays out a certain unwritten script
(depending on the sort of illness, its course and stage) which determines
the possibilities for treatment.
Coping is a different
process of overcoming the chronic illness. This implies behaviour polarized
between avoidance on one hand and vigilance on the other. Avoidance
is shown by the patient who no longer attempts to face up to the stressful
aspects of his illness, which are (apparently) not believed, or the threat
not recognized. Vigilance however is characterized by taking threatening
aspects of the illness extremely seriously and being concerned with these
to an excessive degree. It is unclear which of these two strategies (vigilance
or avoidance) is "more effective".
The many stages of facing-up
and adaptation in the seriously ill can be clearly seen for example
in dialysis patients. Baldamus (1986) listed factors which can assist adaptation
in chronic dialysis patients:
| |
Recognition
of the disease |
| |
Desire to continue
living |
| |
Discipline (diet,
fluid intake, medication, dialysis regime) |
| |
Rehabilitation
in a career |
| |
Social activities |
| |
Family relationships |
| |
Psychological
acceptance |
It should not be forgotten
when caring for the chronically sick, that secondary unconscious processes
can run parallel to the disease, and serve to maintain the disease.
These tendencies are encouraged by those social structures which maintain
a high degree of social security.
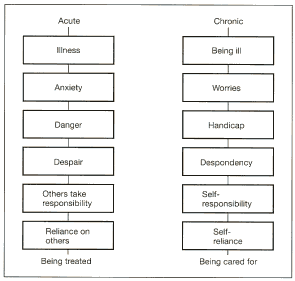
The differences between
acute and chronic sickness (F. Hartmann, 1986)
In principle, it must be presumed
that all chronic illnesses are accompanied by secondary gain. This
increases with increasing conveniences (freedom from unpleasant work, special
holidays, different status) that are conceded in connection with the illness.
| top |
 |
|
The doctor and the
chronic patient
There are very basic differences
between acute and chronic illness. They therefore need to
be approached by different methods of leading discussions and strategies
of treatment. Hartmann differentiated between acute illness and chronic
being-ill, as shown in the Figure.
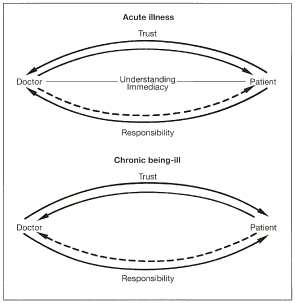
The differing division
of trust and responsibility between the doctor and the acutely or chronically
patient (F. Hartmann, 1986)
In view of the varying natures
of acute illness and chronic illness, the sharing of trust and responsibility
is completely different. While acute illness is characterized by conferring
responsibility and trust to others, in chronic illness, self-responsibility
and trust in one's own capabilities are needed (see Figure).
Further points of view
have to be taken into account in the care of the chronically sick:
| |
The
chronically ill patient often shows a particularly intense need for
information. This can mean that he becomes an "expert" over the course
of his illness. This expertise must be accepted as part of the adaptation
process, and it can be a positive element in patient care. |
| |
The chronically
sick patient becomes extremely sensitive to claptrap, half-truths and
deceptive hopes. These are often the real cause of wandering from one
doctor to another. Werner Zenker, who has chronic asthma, writes about
learning to live with asthma as follows: "Can you protect yourself from
bad experiences with doctors? A prerequisite is not to have excessive expectations!
Only when you are convinced that your doctor is not pretending to be a
miracle worker, but rather your partner in the disease process, and only
after many concrete observations, can you decide if you have made a good
choice". |
| |
Chronic illness
can become a tool which can be used consciously or unconsciously
to suit one's own purposes: to control the spouse, the doctor, the Health
Service, or what goes on around one. |
Almost every chronic patient
leaves traditional medicine and uses other methods. The doctor should not
be personally upset about this, but accept it as a learning process which
is necessary for his patient, nevertheless taking care to factually inform
him of the dangers of any particular method of treatment. Hartmann summarized
the responsibilities and the role of the doctor in the care
of chronically sick patients as follows:
| 1. |
Prevention
and overcoming of crises |
| 2. |
Control of
the symptoms of disease |
| 3. |
Working out
of ways of behaviour and treatment plans |
| 4. |
Organizing
protection from social isolation |
| 5. |
Preparations
for changes or relapse of the disease |
| 6. |
Encouragement
and help to behave and cope like a conditionally healthy person |
| 7. |
Finding out
about help to which he is entitled: social assistance, money, work,
rehabilitation |
| 8. |
Creation of
a working doctor-patient relationship |
In the ideal case, the doctor
will be able to "assist a patient to move from the status of chronic illness
(even temporarily) into that of qualified healthiness" (Hartmann).
| Guide-lines for the care
of chronically ill patients |
| 1. |
Being-ill
chronically is not at all the same as acute illness. |
| 2. |
More emphasis
has to be placed on care than on treatment. |
| 3. |
Processes for
coping (defense mechanisms, overcoming strategies) must be taken into account.
It is most important to strengthen the patients' self-responsibility
and self-reliance. |
|
| top |
 |
| previous page |
 |
| next page |
 |
|
|
Linus
Geisler: Doctor and patient - a partnership through dialogue
|
|
©
Pharma Verlag Frankfurt/Germany, 1991
|
|
URL
of this page: http://www.linus-geisler.de/dp/dp20_illness.html
|
|